Consider prednisone carefully if you’re exploring treatment options for pancreatitis. While prednisone can suppress inflammation and modify immune responses, its use in pancreatitis management remains contentious. We evaluate the benefits and risks, focusing on how this powerful corticosteroid interacts with the complex mechanisms of pancreatic inflammation.
Prednisone’s potential to reduce inflammation might seem beneficial. However, pancreatic inflammation differs from inflammatory conditions where prednisone shines. Understand that the underlying causes of pancreatitis, such as gallstones or alcohol abuse, aren’t directly addressed by prednisone. Instead, the drug primarily masks symptoms by damping down the immune system.
Examine studies on autoimmune pancreatitis where prednisone finds legitimate use. This rarer form sees the immune system attacking the pancreas directly. Here, prednisone can induce remission by halting this autoimmune response. Contrast this with acute pancreatitis from gallstones, where removing the stones constitutes the primary treatment, and prednisone plays little to no role.
Be aware of potential side effects. Prednisone’s prolonged use can lead to serious complications, like increased risk of infection, bone thinning, and glucose intolerance. Discuss these risks openly with your doctor. If you have existing conditions like diabetes or osteoporosis, the potential downsides may outweigh the benefits.
- Prednisone for Pancreatitis: A Concise Guide
- Is Prednisone Ever Used for Pancreatitis?
- Autoimmune Pancreatitis (AIP) and Prednisone
- Why Prednisone Isn’t Commonly Used for Other Types of Pancreatitis
- Prednisone and Autoimmune Pancreatitis (AIP): What to Know
- Potential Risks and Considerations of Prednisone in Pancreatitis Treatment
- Potential Side Effects to Watch For
- Specific Considerations for Different Types of Pancreatitis
Prednisone for Pancreatitis: A Concise Guide
Consult your doctor promptly regarding Prednisone use for pancreatitis. It’s primarily beneficial in autoimmune pancreatitis (AIP), a rare form where the body attacks its own pancreas. Prednisone’s anti-inflammatory action helps manage this condition, preventing further damage.
For AIP, doctors typically prescribe a high starting dose of Prednisone (e.g., 40-60 mg daily), which gradually tapers down over weeks or months as symptoms improve. Monitor your symptoms carefully and communicate any changes to your healthcare provider during this tapering process.
Prednisone is generally not used for acute pancreatitis caused by gallstones or alcohol abuse. In these cases, the focus is on supportive care (fluids, pain management) and addressing the underlying cause.
Be aware of potential side effects. Common ones include weight gain, increased appetite, mood changes, and elevated blood sugar. Long-term use can lead to more serious complications, such as osteoporosis and increased risk of infection. Discuss these potential risks with your physician prior to starting the medication.
Regular blood tests are necessary while taking Prednisone. These tests monitor your liver function, blood sugar levels, and electrolyte balance. Your doctor will adjust your Prednisone dose based on these results and your overall response to treatment.
Always inform all your healthcare providers that you are taking Prednisone. This is particularly important before any surgery or dental procedures.
If you experience new or worsening symptoms while taking Prednisone, seek immediate medical advice. Do not stop taking Prednisone abruptly without consulting your doctor, as this can lead to withdrawal symptoms.
Is Prednisone Ever Used for Pancreatitis?
Prednisone sometimes plays a role in treating pancreatitis, but its application is specific and not a standard treatment. Doctors primarily consider it when pancreatitis has an autoimmune origin, such as in autoimmune pancreatitis (AIP). AIP is a rare form of pancreatitis where the body’s immune system mistakenly attacks the pancreas.
Autoimmune Pancreatitis (AIP) and Prednisone
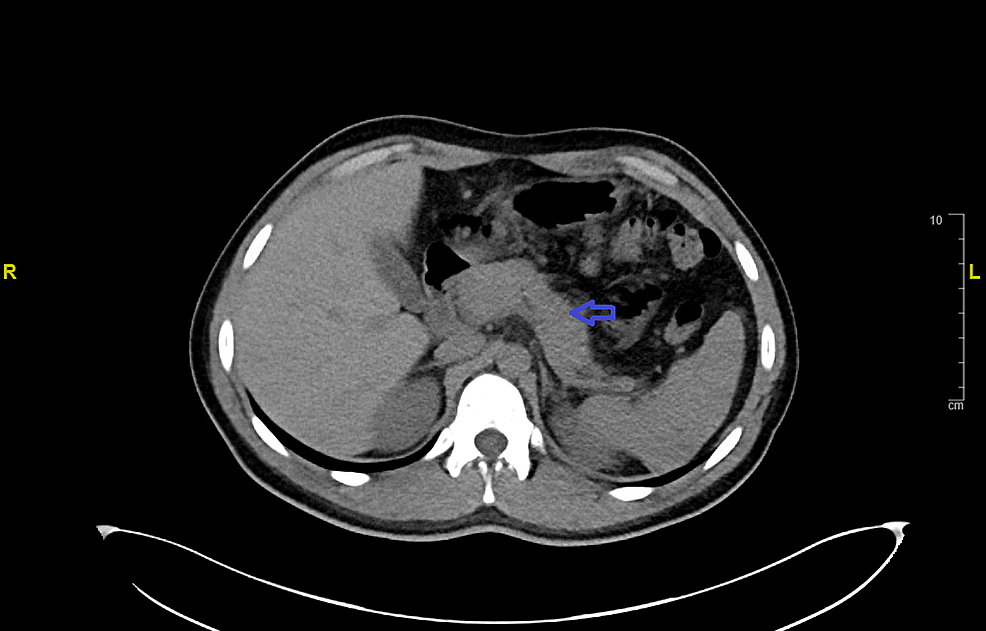
Prednisone can be beneficial for AIP because it suppresses the immune system, reducing inflammation and damage to the pancreas. Diagnosing AIP requires specific tests, including imaging studies (CT scans, MRI), blood tests to check for elevated IgG4 levels, and sometimes a biopsy of the pancreas. You will likely undergo multiple tests before a doctor decides if AIP is the underlying cause of your condition.
The usual initial dose of prednisone for AIP is relatively high, such as 40-60 mg per day. This dosage can be adjusted by a doctor based on the response and side effects. The goal is to induce remission, after which the dosage is gradually tapered to prevent relapse. Long-term use of prednisone always requires careful monitoring due to potential side effects.
Why Prednisone Isn’t Commonly Used for Other Types of Pancreatitis
For most other forms of pancreatitis, such as those caused by gallstones or alcohol abuse, prednisone is generally not the first-line therapy. These types of pancreatitis require different approaches, like removing gallstones or managing alcohol withdrawal. Prednisone is not effective in treating these conditions, and it could potentially worsen the situation due to its side effects. Doctors often prescribe other medications, like pain relievers and anti-nausea medications, as the primary treatment options.
Prednisone and Autoimmune Pancreatitis (AIP): What to Know
Prednisone is a primary treatment for Autoimmune Pancreatitis (AIP) because it effectively suppresses the autoimmune response that causes inflammation in the pancreas.
- Expect your doctor to typically prescribe an initial dose of prednisone ranging from 30 to 40 mg daily. They will adjust this dose based on your response and disease severity.
- Pay attention to symptom improvement, such as reduced abdominal pain and jaundice, which usually occurs within 2-4 weeks of starting prednisone. Consistent monitoring is vital.
- Be aware of common side effects, including weight gain, mood changes, increased blood sugar, and elevated blood pressure. Your doctor should monitor these throughout your treatment.
Because long-term prednisone use can lead to significant side effects, doctors aim to taper the dosage slowly once the AIP is under control.
- Plan for a tapering schedule, which may last several months to a year. A gradual reduction minimizes the risk of relapse.
- Understand that some individuals may require maintenance therapy with a low dose of prednisone or other immunosuppressants, like azathioprine or 6-mercaptopurine, to prevent recurrence. Discuss this with your healthcare provider.
Consider these points regarding relapse and further management:
- Know that AIP can recur even after successful treatment. Be vigilant for symptoms returning.
- If a relapse occurs, prednisone is often used again. Your doctor will determine the optimal dose and duration.
- Discuss alternative treatments with your doctor if you cannot tolerate prednisone or if relapses are frequent. Rituximab is an option for some patients.
Keep in mind that prednisone, while helpful, doesn’t address the underlying cause of AIP, only its symptoms. Lifestyle changes, such as a healthy diet and avoiding alcohol, complement medical treatment.
Potential Risks and Considerations of Prednisone in Pancreatitis Treatment
Before using prednisone for pancreatitis, discuss your complete medical history with your doctor. Prednisone can interact with existing conditions and medications, potentially causing adverse effects. Consider alternatives when treating pancreatitis, as prednisone’s role is not yet definitively established.
Monitor blood sugar levels closely. Prednisone often elevates glucose, a particular concern for individuals with diabetes or pre-diabetes. Adjustments to diabetes medication may be necessary while on prednisone.
Potential Side Effects to Watch For
Be aware of potential side effects such as mood changes (irritability, anxiety, depression), weight gain, increased appetite, fluid retention, and increased susceptibility to infections. Immediately report any unusual symptoms to your healthcare provider.
Long-term prednisone use can weaken bones (osteoporosis) and increase the risk of fractures. Discuss preventative measures with your physician, like calcium and vitamin D supplements, or bone density screenings, if prolonged treatment is anticipated.
Specific Considerations for Different Types of Pancreatitis
Prednisone use requires careful evaluation. In cases of acute pancreatitis potentially caused by autoimmune disorders, such as autoimmune pancreatitis (AIP), it might be appropriate. However, use in non-autoimmune-related acute pancreatitis requires further research and discussion with your specialist. For chronic pancreatitis, carefully weigh the risk-benefit ratio. Consider the potential of long-term adverse effects against the potential of symptom relief. Discuss alternative therapies, such as pain management strategies and lifestyle modifications, as first-line approaches before considering prednisone for chronic conditions.